Standards for Prostate Biopsy
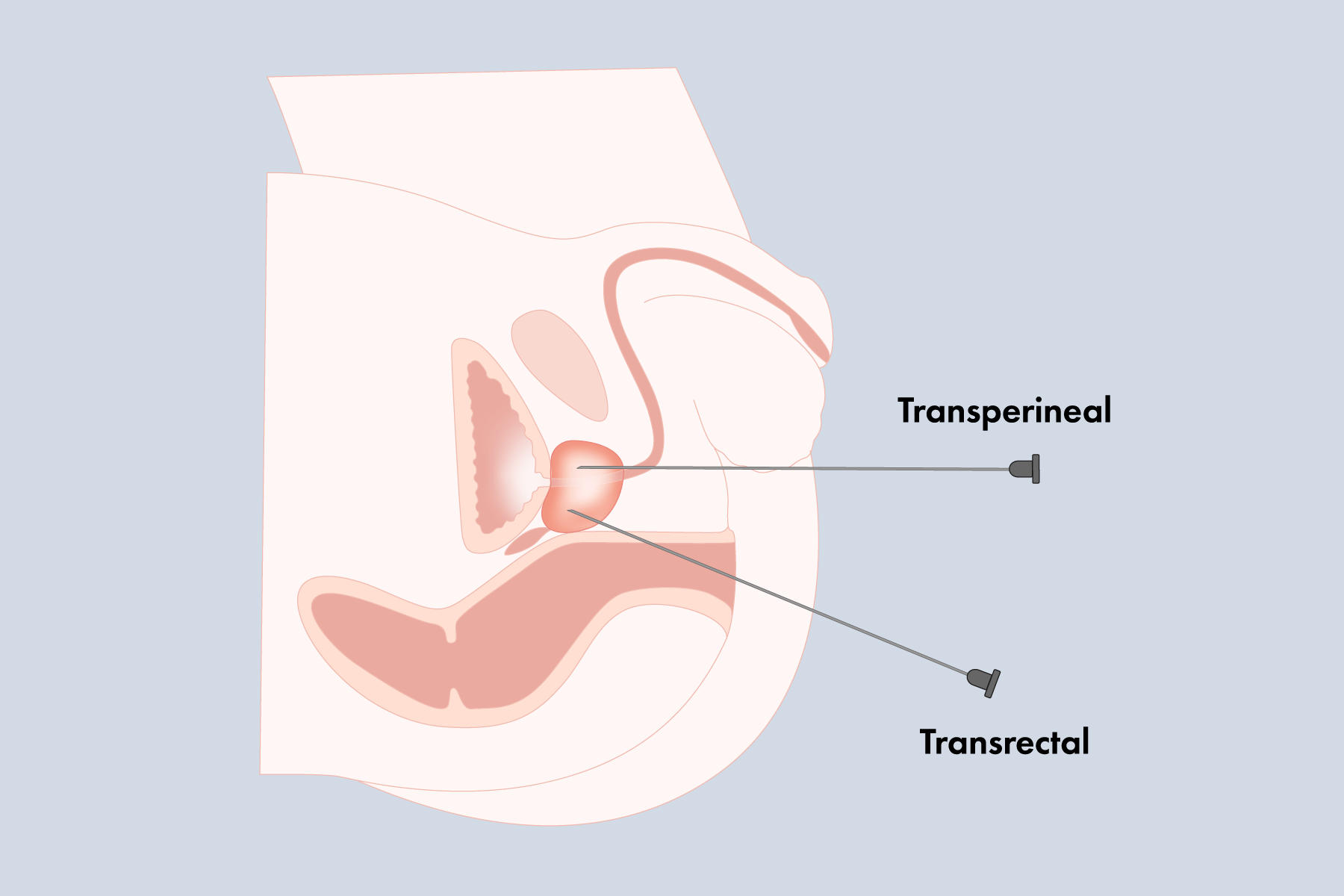
Prostate cancer is the most commonly diagnosed cancer amongst men. It is estimated that over 2 million biopsies are performed annually.1 Because the prostate’s anatomical location lends itself well to the transrectal pathway, it has remained the favoured route for decades.1 Typically, an abnormal digital rectal exam and/or elevated PSA level is a one way ticket to a systematic transrectal biopsy. Guided by ultrasound imaging, 10-12 random samples are taken using a hollow needle. Since the appearance of cancer on ultrasound imaging is pretty ambiguous, this method is considered “blind” as doctors try to sample the prostate in a systematic way.2 Currently the 10-12 core systematic transrectal biopsy is the standard for detecting prostate cancer (PCa), despite the fact that this method underestimates PCa incidence with a high false negative rate of up to 49%.3 Magnetic resonance imaging (MRI) offers an alternative diagnostic pathway in men with a clinical suspicion of cancer. Due to its superiority in differentiating between cancerous and normal tissue, the use of MRI as a triage test can not only improve detection rates of clinically significant cancer, but also prevent unnecessary biopsies.2 Whether systematic or MRI-targeted, biopsies may be performed via transrectal or transperineal approaches.1
The Transrectal Approach
The transrectal approach is favoured amongst doctors for its convenience, short learning curve and low cost. A systematic freehand transrectal biopsy (Fig 1.) may be performed in-office in as little as 10 minutes. Because the procedure is often done under local anaesthesia, this eliminates the need for specialized staff, a dedicated operating room and specialized equipment.1 Transrectal biopsies are considered a “dirty” procedure because the needle passes through the rectal wall, where each pass poses a risk to inoculate the prostate with rectal bacteria. To prevent infection, an enema and prophylactics, typically fluoroquinolonesFluoroquinolones are a type of carbapenem which is a highly effective class of antibiotics typically used to treat resistant bacterial strains.4, are administered prior to biopsy.1 However, fluoroquinolones have a major drawback in that its routine use may be developing the growth of antibiotic resistant bacteria and therefore making prophylactics less effective.1 Advances in MRI-targeted biopsy have addressed the issue of inaccuracy and a high false negative rate, but there is still concern for potential complications like rectal bleeding, fever, sepsis, hematuria and acute urinary retention.3
The Transperineal Approach
“The rate of sepsis post-transperineal biopsy is nearly 0%, which is 40 to 70 times less than that of transrectal.”5
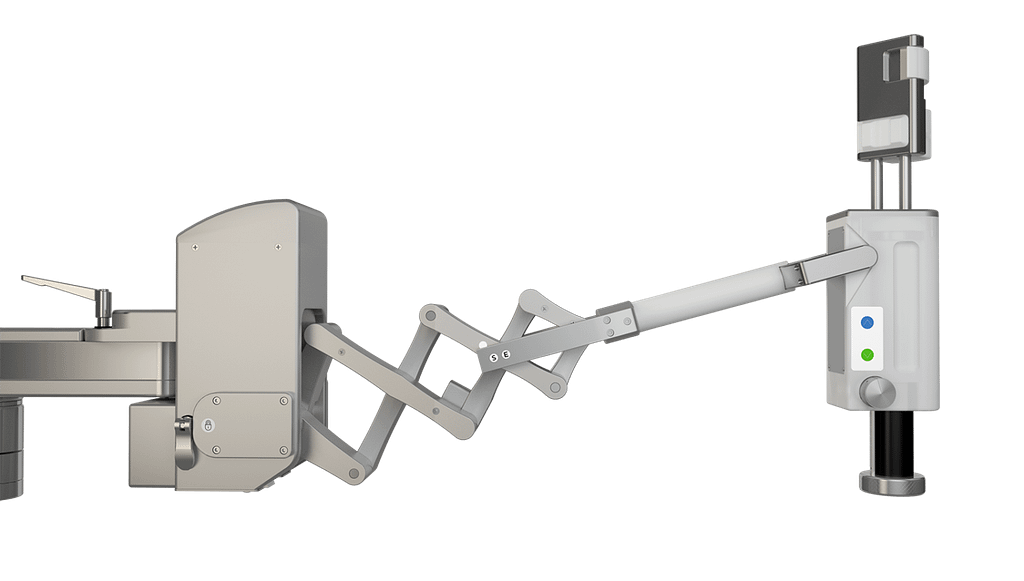
Compared to transrectal, transperineal biopsies are considered “clean” because the needle passes through the perineum, rather than the rectum. This eliminates the need for fluoroquinolone prophylactics.1 The rate of sepsis post-transperineal biopsy is nearly 0%, which is 40 to 70 times less than that of transrectal.5 Unfortunately, this has only benefited a minority of cases as transperineal biopsies are typically reserved for patients undergoing a repeat biopsy (either for active surveillance or a rising PSA level) after a negative transrectal biopsy.5 It is also considered a safer option for those who are prone to infection, have diabetes, prostatitis or urinary catheterization.3 There has been some resurgence in clinical practice, but mainly for its superiority in targeting apical and anterior regions.6 Despite these major advantages, the transition to transperineal biopsies has been slow due to the perceived need for general anesthesia, inconvenience and higher cost.6 Compared to transrectal biopsy, which can be performed in-office under local anesthesia, a transperineal biopsy is often done under general anesthesia, which requires additional time, specialized staff and a dedicated operating room.1 Contrary to the belief, transperineal biopsies do not have to be done this way. The use of local anesthesia is an accessible and cost-friendly option that benefits both clinics and patients. As such, it is becoming more widely accepted for transperineal biopsies because it can be performed in office and is equally tolerable as a transrectal biopsy.6 Traditionally, the procedure utilizes a brachytherapy grid, stabilizer, stepper and bi-plane transducer (Fig 2.). For the majority of clinics that practice standard transrectal biopsies or the even fewer that rely on MRI-targeted biopsies via freehand systems, both cases would have substantial upfront costs in purchasing all of the specialized transperineal equipment.
The Fusion Bx: A Transrectal and Transperineal Solution
1 Grummet, J., Pepdjonovic, L., Huang, S., Anderson, E., & Hadaschik, B. (2017). Transperineal vs. transrectal biopsy in MRI targeting. Translational Andrology and Urology, 6(3), 368–375. doi: 10.21037/tau.2017.03.58
2 Kasivisvanathan, V., Rannikko, A. S., Borghi, M., Panebianco, V., Mynderse, L. A., Vaarala, M. H., . . . Moore, C. M. (2018). MRI-Targeted or Standard Biopsy for Prostate-Cancer Diagnosis. New England Journal of Medicine, 378(19), 1767-1777. doi:10.1056/nejmoa1801993
3 Xiang, J., Yan, H., Li, J., Wang, X., Chen, H., & Zheng, X. (2019). Transperineal versus transrectal prostate biopsy in the diagnosis of prostate cancer: a systematic review and meta-analysis. World Journal of Surgical Oncology, 17(1). doi: 10.1186/s12957-019-1573-0
4 Zowawi, H. M., Harris, P. N. A., Roberts, M. J., Tambyah, P. A., Schembri, M. A., Pezzani, M. D., … Paterson, D. L. (2015). The emerging threat of multidrug-resistant Gram-negative bacteria in urology. Nature Reviews Urology, 12(10), 570–584. doi: 10.1038/nrurol.2015.199
5 Grummet, J. P., Weerakoon, M., Huang, S., Lawrentschuk, N., Frydenberg, M., Moon, D. A., … Murphy, D. (2014). Sepsis and ‘superbugs’: should we favour the transperineal over the transrectal approach for prostate biopsy?. BJU International, 114(3). doi: 10.1111/bju.12536
6 Patel, P. (2020, February). The case for transperineal prostate biopsy vs. the transrectal approach. Urology Times, 48(2), 16–17.