What is image registration?
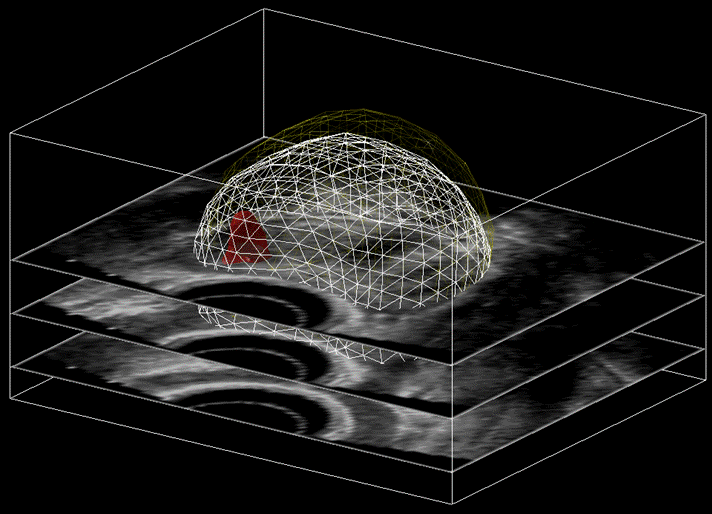
Perhaps the most crucial step of prostate fusion biopsy is that of registration. It allows different sets of data, that have been captured using separate technologies, to be compared and contrasted. Image registration refers to the process of aligning images so that comparable characteristics can be easily related to one another. During this process, points from one image are mapped to analogous points on another image.1
In the field of prostate fusion biopsy, registration refers to the process in which a series of MR images are fused to a 3D ultrasound construct by overlaying the two shapes. Prior to biopsy, a radiologist segments the MR images by contouring the shape of the prostate and placing fiducial points on easily identifiable landmarks.1 During the biopsy, a live ultrasound sweep generates multiple segments of images to create a 3D construct. The common fiducial points are then matched to one another. Fusion is completed using a software registration algorithm typically using one of two techniques: rigid or non-rigid (elastic). The algorithm may be specific to each device; as such, image registration techniques vary between fusion biopsy systems.2
How does the quality of the registration affect targeting accuracy?
Image registration is integral to successful execution of the eponymous fusion step of the fusion biopsy procedure — the process by which previously acquired MRI and live ultrasound images are superimposed or ‘fused’ to each other. This fusion process includes regions of interest (ROI), or areas where there is suspicion of cancer, identified in MRI to be transposed onto the live ultrasound. If the corresponding fiducial points from the MRI and ultrasound images are not adequately identified and paired, the 3D visual volume constructed, along with the location, shape and size of the ROI, will not be as accurate.1 For this reason, image registration is possibly the most important step of fusion biopsy.
What are the image registration methods used for fusion biopsies?
There are two main image registration methods used in fusion biopsy: rigid registration and non-rigid (or elastic) registration.
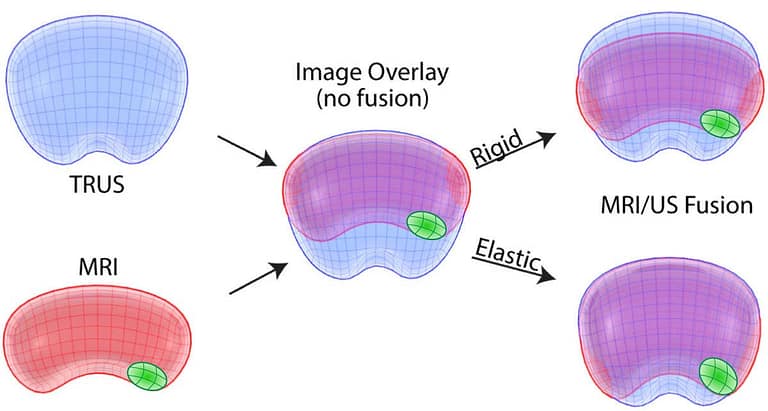
- Rigid registration does not change the images acquired from MR or ultrasound, thus preserving the internal architecture of the prostate. The MRI is overlaid on the TRUS image, where each image set is limited to rotational and translational transformations.2 Although it is not uncommon for the shape and local deformation to differ between MRI and TRUS, rigid registration cannot account for these differences.3 This offset can disproportionately impact location of the overlaid regions of interest and targeting success.1 The operator may account for any misalignment by manually adjusting internal fiducials or probe depth and/or pressure during targeting.3 This requires a “cognitive optimization” of the registration and thus relies more heavily on the operator to make the proper corrections.4 If the MRI segmentation and TRUS volume cannot be sufficiently matched, elastic registration is required to force corresponding data sets together.2
- Non-rigid (elastic) registration changes the images acquired by stretching one of the image volumes to match the other. This is done through pairing corresponding fiducial points within the MR and US volumes.2 These fiducial points often indicate the boundary of the prostate within different segments and along different axes.1 The key difference between rigid and non-rigid registration, is that non-rigid can account for differential local deformations between MRI and US. These deformations may be caused by a TRUS probe, time lapsed between the MRI and the procedure and warping/scale changes.3 However, as images are stretched and moved, so is the data acquired. Some non-rigid registration algorithms may compromise data integrity.1
Focal Healthcare’s Fusion Bx: Intelligent non-rigid registration
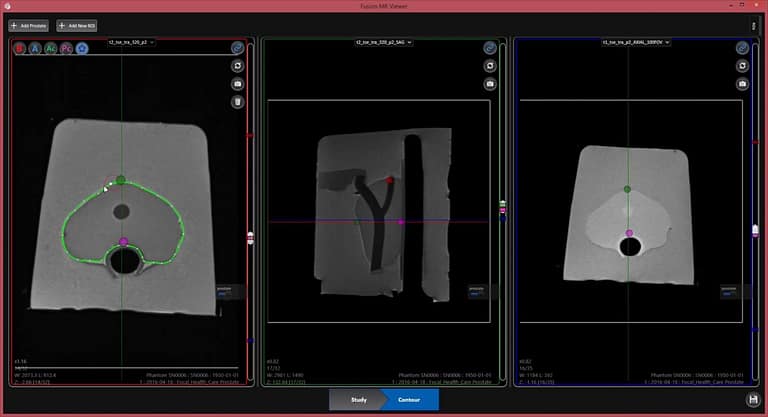
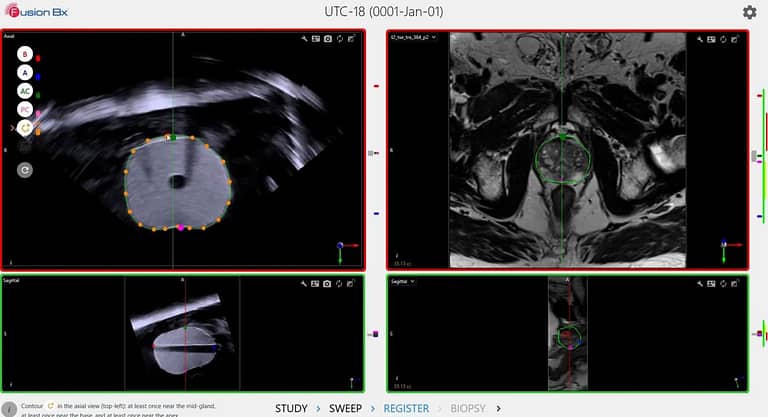
The ideal fusion platform utilizes both elastic and rigid registration, which offers users the flexibility to adjust registration and optimize targeting.2 With rigid registration, image alignment can be highly operator dependent, whereas non-rigid (or “elastic”) registration depends heavily on the algorithm used and the quality and quantity of data points. These fiducial points, identified by the user, may be represented as the number of segments, axes and internal landmarks.1 The Fusion Bx uses easily identifiable landmarks to align images, while the device’s non-rigid registration component automatically segments the prostate and deforms each slice using a few simple contours. Additionally, the Fusion Bx’s automatic motion compensation adjusts for patient movement and maintains image coupling, allowing procedures to continue uninterrupted.
Which registration method is the best choice for my practice?
A systematic review completed by Radboud University Medical Center compared the detection rates of rigid and non-rigid registration for any or clinically significant prostate cancer (csPCA). Overall, the detection rates from cognitive fusion (rigid registration) were highly inconsistent, whereas the majority of fusion (rigid and elastic registration) studies reported similar rates of csPCA.4
As such, experience may play a significant role in determining which registration method will work best for a particular practice. While examining co-registration accuracy, researchers found that “the worst results were obtained by the least experienced operators”.5 As doctors with minimal experience may be more reliant on software guidance, they may only target a ROI strictly where the software indicates it to be. With rigid registration, the unaccounted differences in shape may cause targets to be offset and therefore, the operator must make corrections cognitively. This requires extensive knowledge and experience with the imaging system, whereas the guided workflow and automated segmentation of elastic registration offers significant benefits to beginners.5
Ultimately, users should recognize the limitations of both rigid and elastic registration, choosing a device that best suits the usability needs of its practice. While rigid registration maintains greater data integrity, non-rigid (elastic) can account for differential deformations of the prostate. Regardless of the algorithm employed, targeting accuracy is dependent on the quality of registration.2 This crucial step has the biggest opportunity for error, arguably more so with rigid, as inaccurate alignment is manually corrected by the operator.4
1 Tay, K. J., Gupta, R. T., Rastinehad, A. R., Tsivian, E., Freedland, S. J., Moul, J. W., & Polascik, T. J. (2016). Navigating MRI-TRUS fusion biopsy: Optimizing the process and avoiding technical pitfalls. Expert Review of Anticancer Therapy, 16(3), 303-311. doi:10.1586/14737140.2016.1131155
2 Kongnyuy, M., George, A. K., Rastinehad, A. R., & Pinto, P. A. (2016). Magnetic Resonance Imaging-Ultrasound Fusion-Guided Prostate Biopsy: Review of Technology, Techniques, and Outcomes. Current Urology Reports, 17(4). doi:10.1007/s11934-016-0589-z
3 Logan, J. K., Rais-Bahrami, S., Turkbey, B., Gomella, A., Amalou, H., Choyke, P. L., . . . Pinto, P. A. (2014). Current status of magnetic resonance imaging (MRI) and ultrasonography fusion software platforms for guidance of prostate biopsies. BJU International, 114(5), 641-652. doi:10.1111/bju.1259
4 Venderink, W., Rooij, M. D., Sedelaar, J. M., Huisman, H. J., & Fütterer, J. J. (2018). Elastic Versus Rigid Image Registration in Magnetic Resonance Imaging–transrectal Ultrasound Fusion Prostate Biopsy: A Systematic Review and Meta-analysis. European Urology Focus, 4(2), 219-227. doi:10.1016/j.euf.2016.07.003
5 Moldovan, P., Udrescu, C., Ravier, E., Souchon, R., Rabilloud, M., Bratan, F., . . . Rouvière, O. (2016). Accuracy of Elastic Fusion of Prostate Magnetic Resonance and Transrectal Ultrasound Images under Routine Conditions: A Prospective Multi-Operator Study. PLoS One, 11(12). doi:10.1371/journal.pone.0169120